The Controversy of Cholesterol and Heart Disease
Dec 14, 2021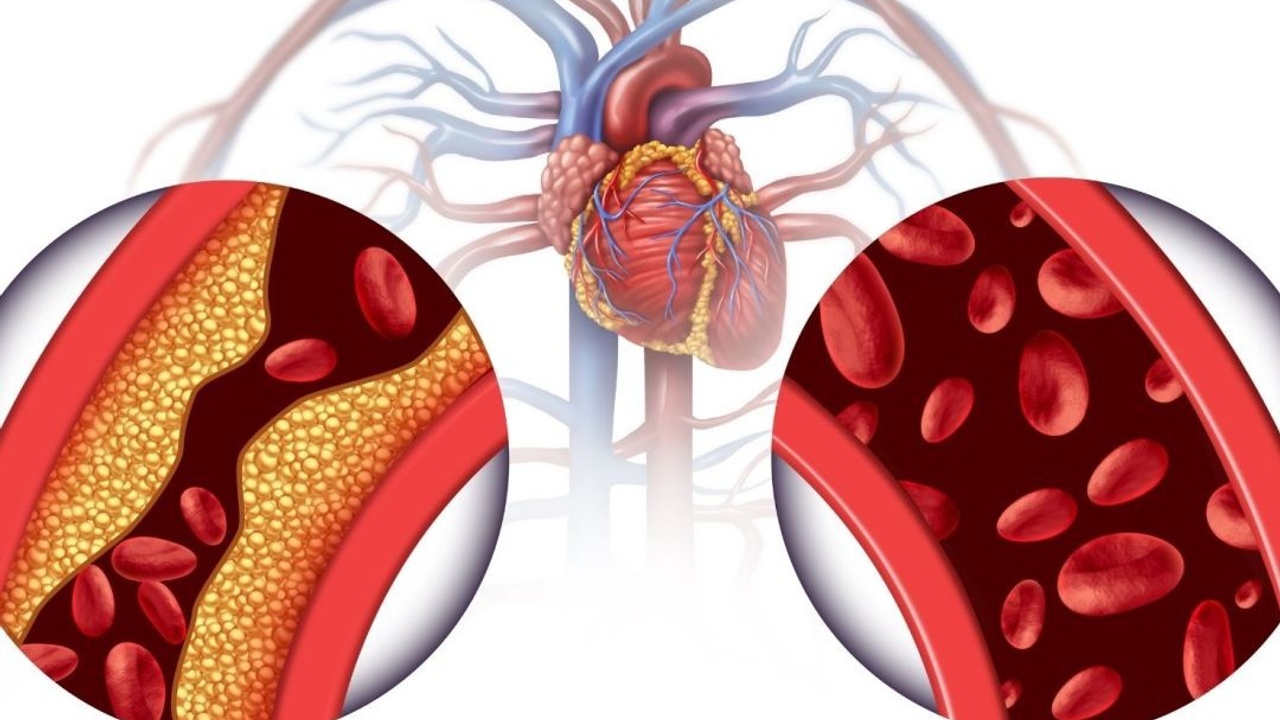
In a recent turn of events, the updated US Department of Agriculture guidelines recommend limiting cholesterol from diets.
A paradigm shift from prior guidelines and the adage that fat = bad. For once, I agree with such policies. Thus, this week at Maximal Being Gut Health, Nutrition, and Fitness, we will explore the controversy of cholesterol and heart disease.
First the Physiology and Biochemistry Behind Cholesterol and Heart Disease
To follow the logic, let’s first establish the chain of events. Heart disease is often the result of plaque formation within arteries (see our Heart Health article here). How does a plaque form?
To develop a plaque, you have molecules called lipids. These further subdivide into:
HDL = high-density lipoproteins (good because they bring lipids from vessels to the liver)
LDL = low-density lipoproteins (bad because they bring lipids from tissues/liver to vessels)
VLDL = very-low-density lipoproteins made of triglycerides (bad)
Triglycerides = from food sources in the form of chylomicrons
Apolipoproteins = part of the above that can elevate lipid signaling and increase risk of disease.
When you eat fat, your intestine via pancreas enzymes (See this article on the Pancreas) and bile, breakdown the fat molecules into tight little packages called chylomicrons, that they can freely pass through your gut lining (See Leaky Gut for an explanation of the gut lining) and into the bloodstream.
The Role of Good and Bad Cholesterol in Heart Disease
Within the bloodstream, particles are continually scanning to look for lipids. Based upon the other parts of your diet, inflammation, stress, etc., will either bring lipids to the liver (via HDL) or the vessels (VLDL and LDL).
Lipids (LDL and VLDL) then arrive onto the lining of the vessels (endothelium) and then oxidize, leading to the generation of pro-inflammatory free radicles. Pro-inflammatory signals then lead to the migration of inflammatory cells called monocytes to the area. Monocytes then turn into little Pacmans called macrophages and eat the oxidized LDL.
With a belly full of fat, these macrophages are then foam cells. Once too complete, the foam cells diet, releasing more inflammation, attracting smooth muscle cells, which form scar tissue or fibrin cap. Due to the inflammation, the plaque will ulcerate, beckoning more inflammatory cells, platelet, and clot formation to attempt a rescue.
How the Plaque in your Artery Causes a Heart Attack
From here, your body will stoke the fire by again ulcerating, causing inflammation, attracting more cells, forming a more significant clot, narrowing the artery until the artery is so narrow that you cannot deliver blood to the tissue. The tissue then is deprived of oxygen, nutrients, and that is when you get an injury, or in the case of the heart, a heart attack.
Where the Cholesterol and Heart Disease Controversy Began
Naturally, scientists then thought, “fat in leads to fat in the vessels.” However, this is scientific baby talk. The human body is more complicated than that.
At the helm of this multi-decade scientific misadventure was a man named Ancel Keys. Ancel Keys was a scientist who pioneered the “Seven Countries Study,” published in 1963.
In this study, Dr. Keys concluded that high cholesterol in the blood led to heart disease. But the cholesterol and heart disease controversy was that they assumed that dietary fat was the source. As a result, he gains the US government’s attention and subsequently, ignoring other factors such as sugar and processed food intake.
The result was “heart-healthy grains,” sugary cereal, and the obesity epidemic we all know and love today. It is also important to note that in 2017 a white paper was published refuting many of Ancel Keys’ findings.
Cholesterol is Important for Many Functions
So, here we are in 2021, and people are on keto diets, eating fat, and our government no longer recommends limiting cholesterol. Why the paradigm shift?
Cholesterol is a vital building block to cell linings or membranes.
Steroid-based hormones, such as estrogen, progesterone, testosterone, etc., are also made of cholesterol.
Bile, which helps break down fats, is also composed of cholesterol.
Therefore, without them, vital processes related to human survival would not be possible.
Saturated Fat, Cholesterol and Heart Disease Controversy
Hence, limiting your diet of cholesterol and fats may also limit these essential human functions. How much fat is too much, if at all?

As we discussed in our review of the macronutrient Fat (here), several types of fats exist:
Monounsaturated Fat
Polyunsaturated Fat
Saturated Fat
Trans Fat
Generally speaking, saturated fats are from animal sources such as meat and dairy. Despite the present and former USDA guidelines limiting saturated fats, five studies show that the link is not linear.
I agree that increasing polyunsaturated and monounsaturated sources derived from vegetables are “good” for heart health (due to the Mediterranean Diet data), however saturated fats are also needed, and the above studies may not link them to heart disease.
The Role of Inflammation In Heart Disease
As stated above, the role of one’s immune system or inflammation may be necessary for forming heart disease via atherosclerosis (plaques).
In this article published in the Journal of Internal Medicine, Dr. Nicoletti summarizes the literature regarding this principle. As stated:

“A fine modulation of the immune response, aimed at targeting the right epitopes, by immunization or tolerization, and controlling the T cell phenotype, may become a powerful tool in the prevention and treatment of in humans.”
They mean that yes, the immune system, inflammation, and the interaction of these factors play an essential role. Therefore, the limitation of inflammation through the body’s natural mechanisms is necessary, such as taking omega-3 fatty acids, limiting stress via proper sleep, mindfulness, and limiting gut inflammation by adequate nutrition and not eating foreign, pro-inflammatory foods.
Insulin
To that point, eating a diet high in high glycemic carbohydrates may negatively impact the heart via inflammation.
The relationship between glucose fluctuations and the vessels is a complex one, as described in this review.
Generally speaking, insulin resistance leads to more free fatty acids due to the lack of fat breakdown (lipolysis). Excess free fatty acids go to the liver, making apoB a crucial component (above) to VLDL. VLDL then enters the bloodstream in high amounts bringing fat from the tissue to the blood-forming plaques.
Usually, the balance of this process is lipoprotein lipase. Yet, insulin resistance also blocks this enzyme, which can break down the high levels of VLDL.
PPARs
In the 1990s, a vitamin A (really retinoid) based cell molecule called PPAR can significantly assist with fat, glucose metabolism, and inflammation. PPAR-alpha can increase good HDL cholesterol, clearing lipids from the blood. Another PPAR-gamma can enhance insulin sensitivity and lower blood glucose. Both molecules are targets for medications in high cholesterol and diabetes, respectively. Some specific individuals genetically lack or have limited PPAR’s hence why specific individuals do poorly on a ketogenic diet (see our article on the ketogenic diet).
In my opinion, I would not recommend taking fibrates or thiazolidinediones if you do not have a medical need for them. My recommendation is mainly because data regarding PPAR activation have not necessarily panned out to improve heart disease. Instead, knowing your body’s internal PPAR signaling may help with a genetic test’s lifestyle strategy.
Generally speaking, this would be an essential strategy before starting a dietary approach, such as the ketogenic diet. Universally, limiting high glycemic foods and sugar intake may help with PPAR modulation. They are asking more questions about our cholesterol and heart disease controversy.
Mitochondrial Stress and Uncoupling in Heart Disease

Other than PPAR, within the cell, the mitochondria (powerhouse) and nucleus (cell brain) may contribute to plaques’ formation. Mitochondria perform much of our energy generation and, like most things, can be affected by stressors in the diet, toxins in the environment, hormone issues, and psychological stress. Damage to this powerhouse can lead to the generation of pro-inflammatory free radicles, as discussed above.
These free radicles are a vital step in the formation of arterial plaques. A primary molecule preventative of the wheels coming off the wagon is uncoupling protein (UCP), present mostly in brown fat.
UCP has several forms. UCP 1 reduces atherosclerosis. A cousin to this molecule is UCP2, which can cause lower levels of glucose and insulin production. Another molecule, UCP3, can release fatty acids from the mitochondria, thus decreasing the mitochondria’s damage from free radicles.
Ultimately uncoupling protects the mitochondria from cell death, which in the vessels can lead to the fibrin cap, clot formation, narrowing, and heart attacks.
How to Biohack Uncoupling
To access your natural uncoupling, you can perform cold thermogenesis, fasting, menthol topical administration. As stated in our article on Intermittent Fasting (here), one of the primary mechanisms by which fasting can assist is autophagy.

Though not purely due to UCP, fasting does impact the mitochondrion’s ability to resist damage and hence death.
Cold thermogenesis works similarly, and the above study also showed an elevation in UCP for the non-human study participants.
Taking the concept of non-shivering thermogenesis one step further, it appears that PKA signaling menthol, when given topically, can induce the same pathways.
Summary of the Cholesterol and Heart Disease Controversy
Understanding the basic principles of cholesterol signaling and plaque formation is crucial to limiting your heart disease risk. Learn from the mistakes of historical studies, such as the decades-long battle against fat.
Eat fats in the proper amount for your height, weight, sex, age, and activity level. Evaluate yourself for possible genetic issues with fat breakdown before starting a ketogenic approach, and note that such factors may be the source of your lack of response if you choose such a diet.
Limit inflammation and support a healthy immune system by limiting psychological stressors through meditation and mindfulness, getting good quality sleep, and eating real food with low sugar and glycemic impact. If you feel significantly cutting edge, try fasting, cold thermogenesis, and topical menthol to uncouple your fat cells.
Until next time, Maximal Beings, this is Doc Mok, and I am Here to Maximize Your Health.



