Advanced Imaging for Pancreatic Cysts
Oct 16, 2022
Pancreatic cysts fall into a variety of diagnostic categories and can be difficult to differentiate. Knowing the distinct type of cyst a patient has is critical to managing treatment and detecting early signs of cancer. As a result, imaging techniques are currently emerging and being updated to address this issue.
Types of Pancreatic Cysts
There are two main types of pancreatic cysts: neoplastic and nonneoplastic. Non-neoplastic cysts are usually benign and only require treatment if they cause symptoms. On the other hand, neoplastic cysts have a significant potential to become cancerous. Because of this, it is vital for doctors to be able to distinguish between these two types of cysts. Each type has several different subtypes. Among the types of non-neoplastic cysts are:
- Pseudocysts: This type of cyst is typically benign and originates from pancreatitis or trauma. It appears fluid-filled and is usually found adjacent to the pancreas.
- Serous cystadenomas (SCAs): SCAs are also fluid-filled, but they are distinguished by their thick walls. They typically do not develop into cancer but can cause discomfort to the patient if they grow large enough.
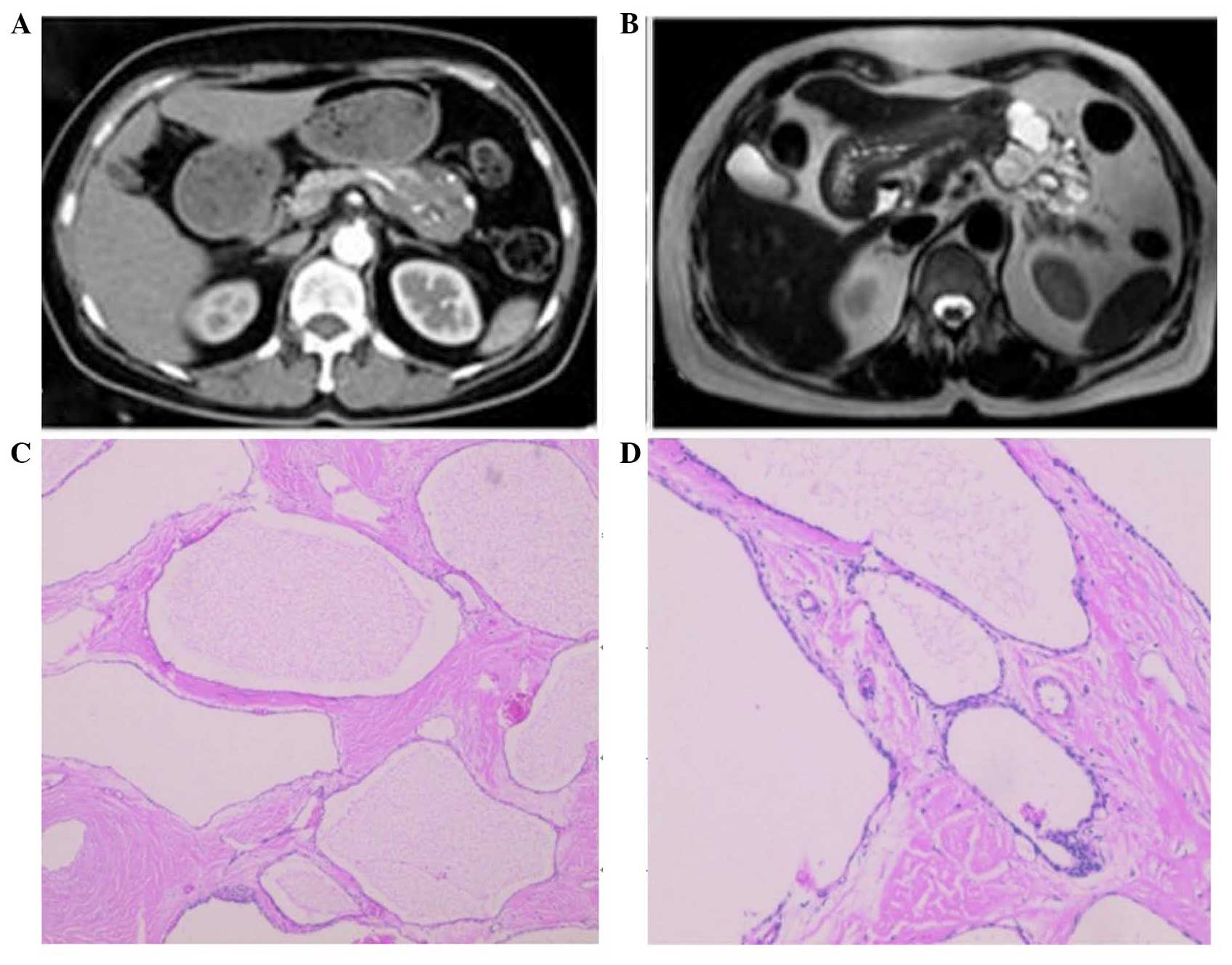
Image from: https://images.app.goo.gl/maWjEZc5smVfSuzq8
Common subtypes of neoplastic cysts include:
- Mucinous cystic neoplasms (MCNs): Typically found in women over the age of 60, MCNs are commonly precancerous. In some cases, larger MCNs have already developed into pancreatic cancer.
- Intraductal papillary mucinous neoplasms (IPMNs): This type of cyst forms in the ducts that lead to the pancreas. It has the potential to become cancerous, and it is the most common type of precancerous cyst.
- Solid pseudopapillary neoplasms: This category of cyst is rare and sometimes cancerous. It is usually found in younger women under 35 years of age.
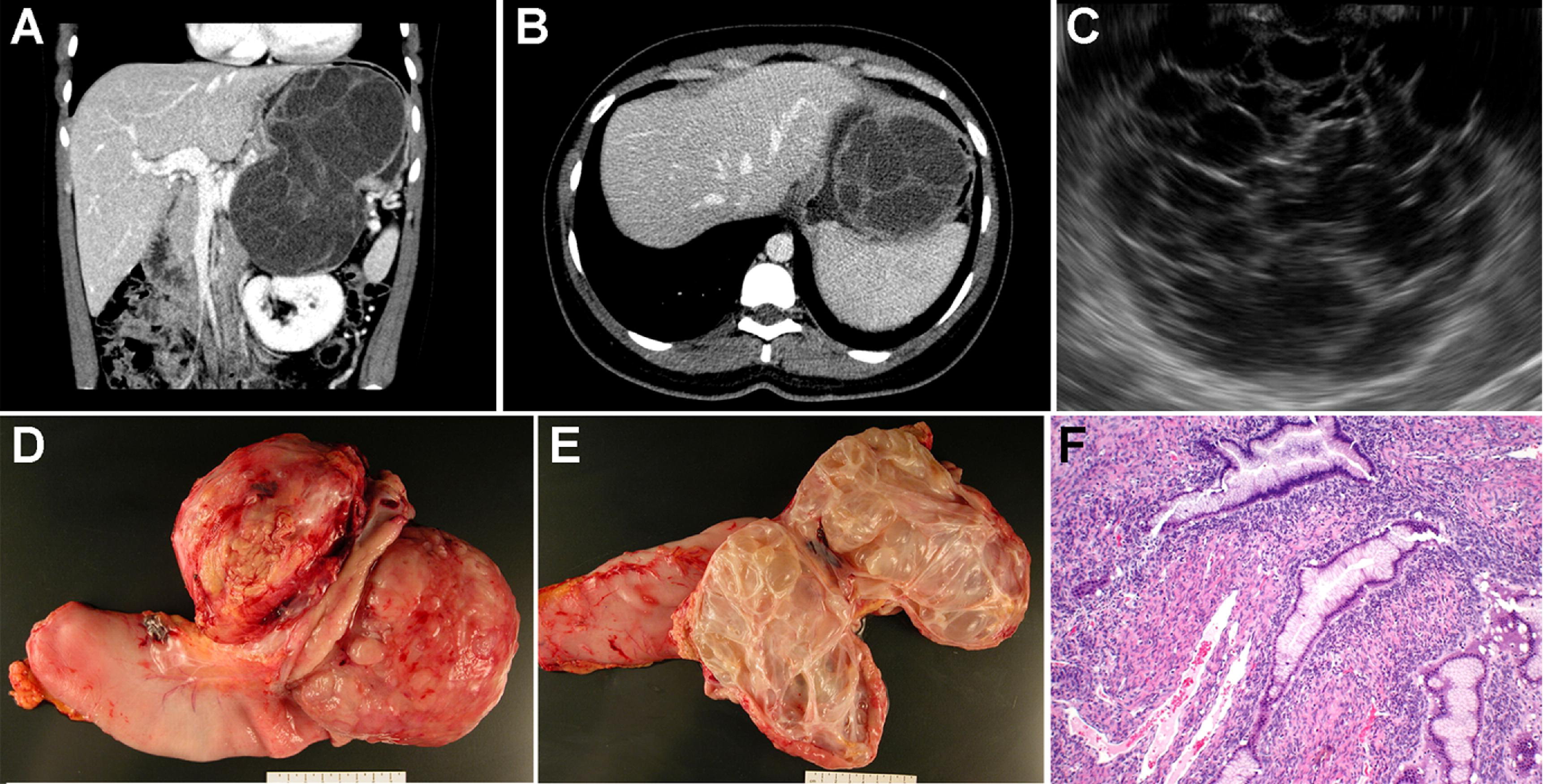
Image from: https://images.app.goo.gl/hR5n2qg9uftmczhb7
Evidently, the various types and subtypes of pancreatic cysts have very different levels of severity, symptoms, and treatment plans. For this reason, it is extremely important for physicians to be able to make correct diagnoses about the type of cyst a patient has. Imaging techniques have been improving in order to help doctors make this distinction.
Contrast-Enhanced Imaging
One main type of imaging used to diagnose pancreatic cysts is contrast-enhanced imaging. This can include contrast-enhanced CT scans and contrast-enhanced endoscopic ultrasound.
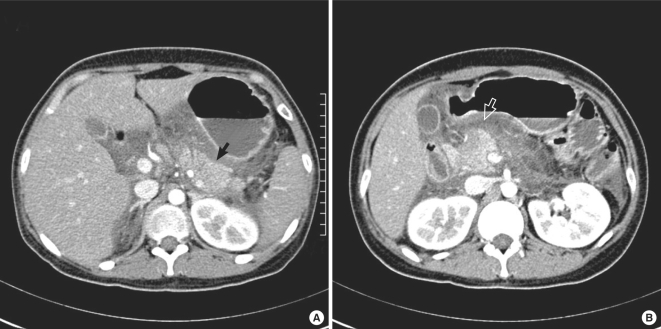 Contrast-enhanced CT (CECT) is most useful for determining the difference between serous cystadenomas, mucinous cystic neoplasms, and intraductal papillary mucinous neoplasms. It differentiates enhancing regions from non-enhancing regions, allowing physicians to better visualize characteristics of various types of cysts. According to a recent study, the diagnostic accuracy of CECT is 72.5 percent. (Image from: https://images.app.goo.gl/Zpn3oxYDYCTwYZGq8)
Contrast-enhanced CT (CECT) is most useful for determining the difference between serous cystadenomas, mucinous cystic neoplasms, and intraductal papillary mucinous neoplasms. It differentiates enhancing regions from non-enhancing regions, allowing physicians to better visualize characteristics of various types of cysts. According to a recent study, the diagnostic accuracy of CECT is 72.5 percent. (Image from: https://images.app.goo.gl/Zpn3oxYDYCTwYZGq8)
 Another type of contrast-enhanced imaging is contrast-enhanced endoscopic ultrasound (CE-EUS). CE-EUS reveals the differences between cystic neoplasias and non-neoplastic cysts by enhancing the walls and other specific features of cystic neoplasms. Fine-needle puncture is typically performed after CE-EUS for further differentiation of subtypes. (Image from: https://images.app.goo.gl/9HeVoWwsdyekF79p9)
Another type of contrast-enhanced imaging is contrast-enhanced endoscopic ultrasound (CE-EUS). CE-EUS reveals the differences between cystic neoplasias and non-neoplastic cysts by enhancing the walls and other specific features of cystic neoplasms. Fine-needle puncture is typically performed after CE-EUS for further differentiation of subtypes. (Image from: https://images.app.goo.gl/9HeVoWwsdyekF79p9)
Elastography
Elastography is a type of imaging that determines the stiffness of a specific tissue. The stiffness level can be used to tell whether a pancreatic cyst is benign or malignant. Elastography can also identify pancreatitis and patients with high risk for developing pancreatic cancer.
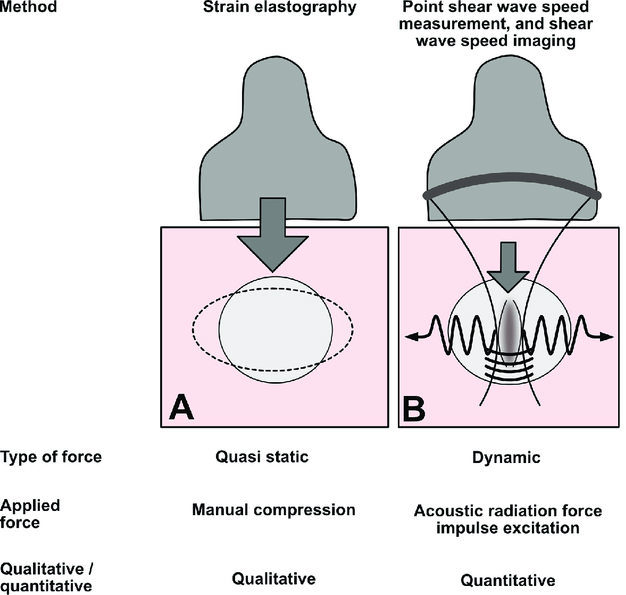
Image from: https://images.app.goo.gl/mYdUJttHcfYUmfzf6
There are two main types of elastography: strain elastography and shear wave elastography. Strain elastography applies external pressure to a tissue and measures the level of strain on that tissue as a result. Shear wave elastography sends a focused ultrasound from a probe to a tissue. A transverse, or shear wave, is then produced by the tissue. The speed of the shear wave is used to determine the stiffness level of the tissue.
An increased stiffness level is associated with malignant pancreatic cysts and tumors. According to a 2019 study, endoscopic ultrasound elastography can eliminate the possibility of malignancy if the tissue in question is soft. This illustrates the importance of elastography in diagnosing pancreatic cysts.
Endomicroscopy
Confocal laser endomicroscopy is a new technique that is used to tell whether a pancreatic cyst is mucinous or non-mucinous. Mucinous cysts are typically precancerous. In confocal laser endomicroscopy, a small microscopy probe is inserted into the tissue being examined, using endoscopic ultrasound as a guide. The microscopy probe is used to visualize the lining, or epithelium, of the cyst.
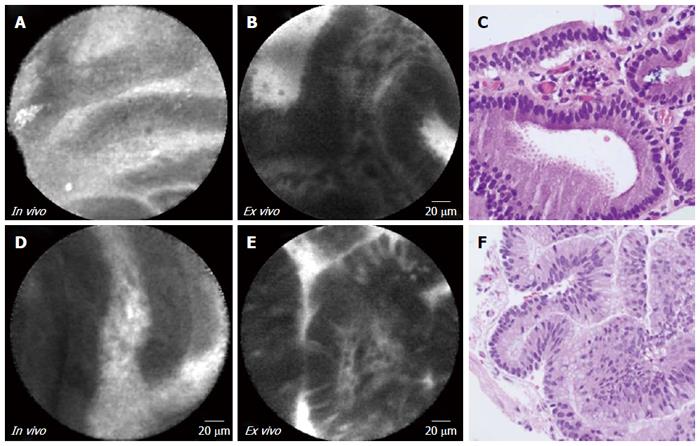
Image from: https://images.app.goo.gl/DpWZr65yoRGsxpeY7
The epithelium can provide useful information about whether the cyst is mucinous or non-mucinous, and it can also be used to diagnose the specific subtype of the cyst. When used with endoscopic ultrasound and fine-needle aspiration, the diagnostic accuracy of confocal laser endomicroscopy is over 90%. This makes it a promising addition to the existing imaging techniques for pancreatic cysts. However, training is required for gastroenterologists to perform and interpret confocal laser endomicroscopy.
Summary
Pancreatic cysts fall into two main categories, neoplastic and non-neoplastic, and each of these categories comprises various subtypes. The diversity in types of pancreatic cysts implies a diversity in severity and treatment options as well. Consequently, it is important for doctors to be able to easily differentiate between the various types of cysts. Various imaging techniques are emerging and developing to allow for this.
Contrast-enhanced imaging, including CECT and CE-EUS, is one type of imaging that allows for identification of specific subtypes of pancreatic cysts. By enhancing certain regions of the cyst, it provides images that are characteristic to certain categories of cysts.
Elastography is another imaging modality that measures the stiffness of tissues. Elastography is especially useful for determining whether a cyst is malignant or benign, which is a highly important classification.
Finally, endomicroscopy is a relatively new technique that allows for diagnosis of specific subtypes of pancreatic cysts. It uses characteristics of the cyst’s epithelium to determine the specific category it belongs to. When used in combination with endoscopic ultrasound and fine-needle aspiration, endomicroscopy can provide significantly higher diagnostic accuracy.
All of these imaging techniques show promise for improving the accuracy and convenience of diagnosing pancreatic cyst subtypes. As a result, patients can be treated for potentially cancerous cysts earlier and more effectively.




